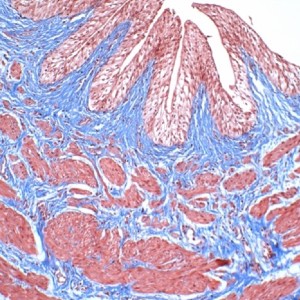
Ureteropelvic junction obstruction in children by polar vessels: histological examination result
Submitted: 17 January 2023
Accepted: 15 May 2023
Published: 30 May 2023
Accepted: 15 May 2023
Abstract Views: 675
PDF: 335
HTML: 8
HTML: 8
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Similar Articles
- Luisella Pedrotti, Barbara Bertani, Gabriella Tuvo, Redento Mora, Luca Marin, Federica De Rosa, Achilles tendon surgery in clubfoot: Are long term sequelae predictable? , La Pediatria Medica e Chirurgica: Vol. 44 No. 1 (2022)
You may also start an advanced similarity search for this article.

 https://doi.org/10.4081/pmc.2023.308
https://doi.org/10.4081/pmc.2023.308




